An electrocardiogram (EKG or ECG) is a diagnostic test that measures the electrical activity of the heart. EKGs are commonly used to diagnose and monitor a variety of heart conditions, including arrhythmias, heart attacks, and heart disease. In this blog post, we will discuss what an EKG is, how it works, and its uses and limitations.
What is an EKG?
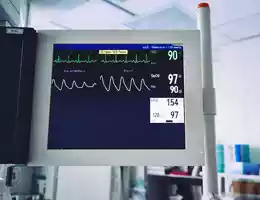
An EKG is a non-invasive test that records the electrical activity of the heart using electrodes placed on the skin. The electrodes are attached to a machine that measures and displays the electrical impulses as waveforms on a monitor or paper printout. The test is painless and takes only a few minutes to perform.
How does an EKG work?
The heart’s electrical activity is generated by specialized cells in the heart’s upper right chamber (the sinoatrial node) that create a small electrical current. This current spreads through the heart and causes it to contract, pumping blood throughout the body. An EKG records this electrical activity by measuring the voltage changes that occur as the current passes through the heart.
During an EKG, the patient lies down and electrodes are placed on the chest, arms, and legs. The machine then records the electrical activity of the heart from multiple angles and displays it as a series of waveforms on a monitor or paper printout.
Uses of EKGs
EKGs are used to diagnose and monitor a variety of heart conditions, including:
- Arrhythmias: EKGs can detect abnormal heart rhythms (arrhythmias) such as atrial fibrillation, ventricular tachycardia, and bradycardia.
- Heart attacks: EKGs can detect the electrical changes that occur during a heart attack, allowing doctors to quickly diagnose and treat the condition.
- Heart disease: EKGs can help diagnose heart disease, such as cardiomyopathy, hypertrophic cardiomyopathy, and pericarditis.
- Other conditions: EKGs can also be used to monitor the effects of medications, pacemakers, and other medical devices on the heart.
Limitations of EKGs
While EKGs are a useful diagnostic tool, they do have some limitations. EKGs cannot detect all types of heart conditions, and abnormal EKGs do not always indicate a serious problem. Other tests, such as echocardiograms, stress tests, and cardiac catheterization, may be needed to confirm a diagnosis.
Additionally, EKGs are only a snapshot of the heart’s electrical activity at a specific moment in time. They may not detect intermittent or fleeting arrhythmias or changes in the heart’s electrical activity that occur over time.
Conclusion
An EKG is a simple, non-invasive test that can provide important information about the electrical activity of the heart. It is a valuable tool for diagnosing and monitoring a variety of heart conditions, but it does have some limitations. Patients should discuss the benefits and limitations of EKGs with their healthcare provider to determine if it is the right diagnostic test for them.