Leg vein ablation is a medical procedure used to treat varicose veins, which are enlarged veins that appear twisted or bulging under the skin. This condition can cause discomfort, pain, and swelling, and can also be unsightly.
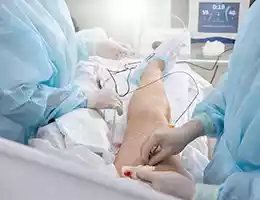
During a leg vein ablation procedure, a small incision is made near the affected vein, and a thin catheter is inserted into the vein. The catheter then delivers energy, such as laser or radiofrequency energy, to the inside of the vein, causing it to heat up and seal shut. This redirects blood flow to healthier veins, improving circulation and reducing the appearance and symptoms of varicose veins.
Leg vein ablation is a minimally invasive procedure that is typically done on an outpatient basis, meaning patients can return home the same day. Local anesthesia is used to numb the area, and sedation may be given to help patients relax during the procedure.
After the procedure, patients may need to wear compression stockings for a few weeks to help reduce swelling and promote healing. Normal activities can usually be resumed within a few days, but heavy lifting and strenuous exercise should be avoided for several weeks.
Leg vein ablation is a safe and effective treatment option for varicose veins, and can improve quality of life for those who suffer from this condition. However, as with any medical procedure, it is important to discuss the risks and benefits with a qualified healthcare provider before making a decision.